A varicose or venous skin ulcer is a sore on your leg that’s very slow to heal, reveal the underlying flesh and usually because of weak bloodcirculation in the limb.
They can last anywhere from a few weeks to years. You may hear a doctor or nurse call them “venous leg ulcers.”
Venous leg ulcers are the most common type of skin ulcer. They mainly occur just above the ankle. They usually affect older people and are more common in women. Venous leg ulcers become more common as you get older. Most are painless but some are painful. Without treatment, an ulcer may become larger and cause problems in the leg. Skin inflammation (dermatitis) sometimes develops around a venous ulcer.They can sometimes lead to more serious problems if you don’t have them treated. But there are steps you can take to prevent them from happening.
Non-venous skin ulcers are less common. For example, a skin ulcer may be caused by poor circulation due to narrowed arteries in the leg, problems with nerves that supply the skin, or other problems. The treatment for non-venous ulcers is different to that of venous ulcers.
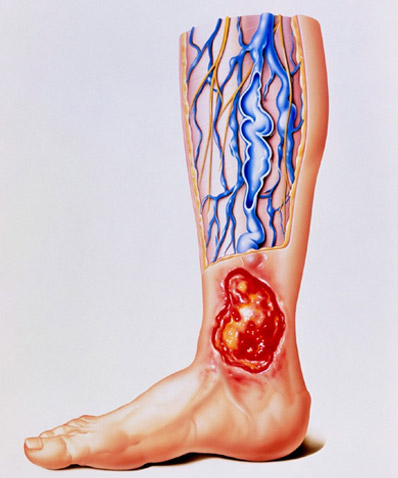
The root of the problem is increased pressure of blood in the veins of the lower leg. This causes fluid to ooze out of the veins beneath the skin. This causes swelling, thickening and damage to the skin. The damaged skin may eventually break down to form an ulcer.
The increased pressure of blood in the leg veins is due to blood collecting in the smaller veins next to the skin. The blood tends to collect and pool because the valves in the larger veins become damaged by a previous blood clot (thrombosis) in the vein, or varicose veins. Gravity causes blood to flow back through the damaged valves and pool in the lower veins.
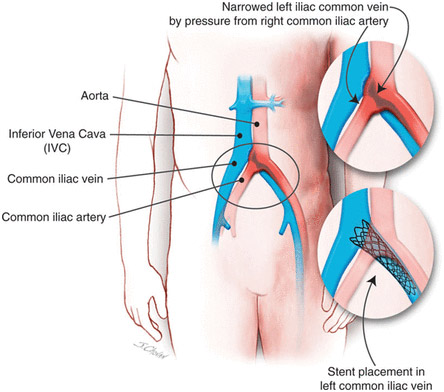
The appearance of a venous leg ulcer is usually fairly typical. It often looks different to ulcers caused by other problems such as poor circulation or nerve problems.
To rule out poor circulation as a cause, it is usual for a doctor or nurse to check the blood pressure in the ankle and in the arm. The ankle blood pressure reading is divided by the arm blood pressure reading to give a blood pressure ratio called the Ankle Brachial Pressure Index (ABPI). If the ratio is low (less than 0.8) it indicates that the cause of the ulcer is likely to be poor circulation (peripheral arterial disease) rather than venous problems. This is very important to know as the treatments are very different. An ABPI may be checked every six months or so to make sure the circulation to the legs remains good.
Certain blood and urine tests may also be done to rule out conditions such as anaemia, diabetes, kidney problems and rheumatoid arthritis, which may cause or aggravate certain types of skin ulcer.In complicated cases you may need to have an ultrasound scan, CT scan or scan to produce a detailed map of the blood circulation in your leg.
The ulcer is dressed in a similar way to any other wound. Typically, a nurse will do this every week or so. The wound is cleaned when the dressing is changed – normally with ordinary tap water. However, an ulcer is unlikely to heal with just dressings. In addition to a dressing, the following treatments help the ulcer to heal.
Compression bandaging
This is the most important part of treatment. The aim is to counteract the raised pressure in the leg veins. This gives the best chance for the ulcer to heal. The common method is for a nurse to put on 2-4 layers of bandages over the dressing. When the bandages are put on, the pressure is put highest at the ankle and gradually less towards the knee and thigh. A support (compression) stocking over the dressing is sometimes used as an alternative but not thought to be as good as bandaging.
The bandages are reapplied every week or so. It is best to put the bandages on after you have raised (elevated) the leg for several hours or overnight (see below). So, make extra effort to keep your leg elevated just before the nurse is due to see you.
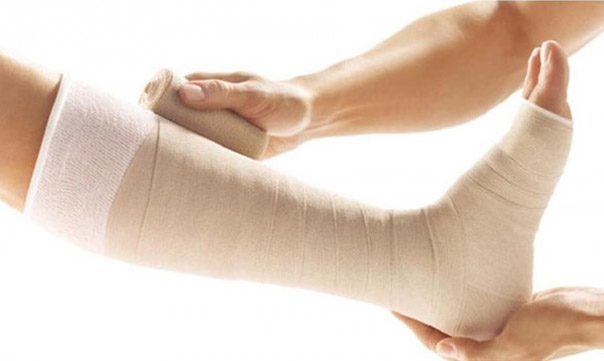
A note of caution: when you have a compression bandage on you should still be able to move your ankle around. Occasionally, the compression is too tight, or it may affect the circulation in the legs. Therefore, take off the bandages if your foot changes colour or temperature, or if you have increasing pain. Then see your doctor or nurse for advice.
Elevation and activity
When you are resting, if possible, try to keep your leg raised higher than your hip. This is particularly important if your leg is swollen. The aim is to let gravity help to pull fluid and blood in the right direction – towards the heart. This reduces swelling in the leg and reduces the pressure of blood in the leg veins. Try to set 3 or 4 periods per day of about 30 minutes to lie down with your leg raised. For example, lie on a bed or sofa with your foot on a couple of pillows. However, do not spend all your time in bed or resting. For the rest of the time, keep as active as you can and do normal activities. If possible, regular walks are good but do not stand still for long periods.
When you sleep overnight, if possible, try to keep your leg raised. You can do this by putting some pillows under the bottom of the mattress. (It may not be possible to sleep like this if you have certain other medical problems or disabilities.)
Endovenous Laser Operation
When the ulcer is caused by venous reflux in the superficial venous system, the problem can be addressed with minimally invasive procedures commonly practiced by Interventional radiologists.
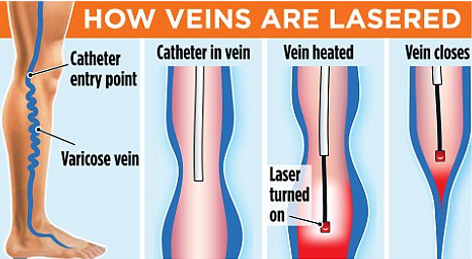
Endovenous Laser Treatment for the elimination of varicose veins responsible for venous ulcer is quickly becoming the gold-standard. Endovenous Laser Treatment uses laser energy, which is simply a highly concentrated beam of light. Medical lasers work by delivering this light energy to the targeted tissue with extreme precision, so as not to affect the surrounding tissue. Lasers have proven their safety and effectiveness through years of use in all types of medical procedures, from eye surgery to dermatology. In the hands of a skilled physician, lasers offer far less risk for complications than conventional surgery.
In endovenous laser treatment, a thin fiber is inserted into the damaged vein through a very small entry point in the skin. A laser light is emitted through the fiber, as the fiber is pulled back through the vein, it delivers just the right amount of energy. The targeted tissue reacts with the light energy, causing the vein to close and seal shut. The veins that are closed are superficial veins that handle less than five percent of the body’s blood flow. The blood is automatically routed to other, healthy veins.
The procedure is minimally invasive and requires no general anesthesia. Only local anesthetic is used to numb the area where the physician is working. Patients are encouraged to walk immediately after the procedure and can resume normal activities the same day.
Other treatments
In some people, other conditions such as anaemia, poor nutrition, swelling of the legs and other medical problems may mean that the skin has less chance of healing well. Other treatments may be needed to help heal a venous leg ulcer – for example:
- Try to stop smoking if you are a smoker. The chemicals in cigarettes may interfere with the skin healing.
- Antibiotic medicines are sometimes advised for short periods if the skin and tissues around the ulcer become infected.
- Painkillers can be taken if the ulcer is painful.
- Skin care. The skin around an ulcer is often inflamed or scaly. Your doctor or nurse may advise on a cream to reduce inflammation if necessary.
- Dietary advice if your diet is not very good. Also, if you are overweight then losing some weight may help. Obesity is a risk factor for developing venous leg ulcers.
- Iron tablets or other treatments if you are anaemic.
- Pentoxifylline improves blood circulation and you may be offered this medicine to promote healing of the ulcer.
- Hyperbaric oxygen (oxygen delivered at high pressure) is sometimes used when facilities are available.
- A skin graft may be advised for a large ulcer, or for one that does not heal well.
