Nasopharyngeal angiofibroma (also called juvenile nasopharyngeal angiofibroma) is a histologically benign but locally aggressive vascular tumor that grows in the back of the nasal cavity.Juvenile nasopharyngeal angiofibromas occur almost exclusively in males and usually in adolescence.
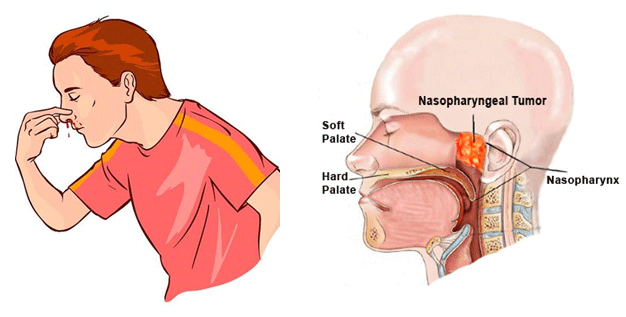
The presentation is typically with obstructive symptoms, epistaxis, and chronic otomastoiditis due to obstruction of the Eustachian tube. Patients may present with life-threatening epistaxis. On examination, it may be seen as a pale reddish blue mass. It is, as the name suggests, very vascular and a biopsy can sometimes be fatal.
Imaging plays an important role in diagnosis, as biopsies should be avoided due to the risk of brisk hemorrhage.
Plain radiograph: Plain radiographs no longer play a role in the workup of a suspected juvenile nasopharyngeal angiofibroma, however they may still be obtained in some instances during the assessment of nasal obstruction, or symptoms of sinus.
CT: CT is particularly useful at delineating bony changes. Typically a lobulated non-encapsulated soft tissue mass is demonstrated centred on the sphenopalatine foramen (which is often widened) and usually bowing the posterior wall of the maxillary antrum anteriorly. There is marked contrast enhancement following administration of contrast, reflecting the prominent vascularity. Extensive bony destruction is usually not a feature, but rather bone is remodelled or resorbed. This feature may be helpful is differentiating from other more aggressive lesions. An intracranial extension can however occur.
MRI: MRI is excellent at evaluating tumour extension into the orbit and intracranial compartments. The presence of prominent flow voids lead to a salt and pepper appearance on most sequences and are characteristic.
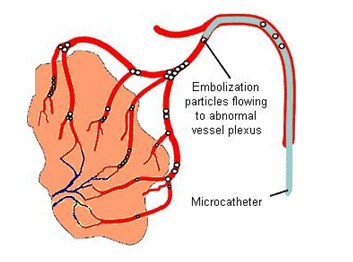
DSA: Angiography, although not essential, is often useful in both defining the feeding vessels as well as in preoperative Embolisation.
Surgical resection (either open or increasingly endoscopic) is the treatment of choice, usually performed with pre-operative embolisation to help with haemostasis. Irradiation may be an option if surgery is not possible or only incomplete resection achieved. In cases where there is skull base involvement a high recurrence rate (up to 50%) has been reported.
Juvenile nasopharyngeal angiofibromas pose a significant bleeding risk for the surgeon due to their highly vascular nature. Pre-operative embolization of juvenile nasopharyngeal angiofibromas can reduce intraoperative blood loss while lessening the risk of massive hemorrhage, shortening operation times, increasing intra-operative visibility, and allowing for easier resection of lesions.