Budd-Chiari syndrome is caused by blood clots that completely or partially block blood flow from the liver. The blockage may occur anywhere from the small and large veins that carry blood from the liver (hepatic veins) to the inferior vena cava.
- Some people have no symptoms, but others experience fatigue, abdominal pain, nausea, and jaundice.
- Fluid may accumulate in the abdomen, the spleen may enlarge, and sometimes severe bleeding occurs in the esophagus.
- Doppler ultrasonography can detect narrowed or blocked veins.
- Drugs may be used to dissolve or decrease the size of the clot, or a connection may be made between veins to allow blood to bypass the liver.
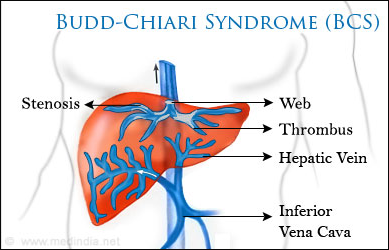
Budd-Chiari syndrome usually occurs when a clot narrows or blocks the hepatic veins, which carry blood out of the liver.
Because blood flow out of the liver is impeded, blood backs up in the liver, causing it to enlarge. The spleen may also enlarge. This backup of blood (congestion) causes blood pressure in the portal vein (which carries blood to the liver from the intestines) to increase. This increased pressure, called portal hypertension, can result in dilated, twisted (varicose) veins in the esophagus (esophageal varices). Portal hypertension, plus the engorged and damaged liver, leads to fluid accumulating in the abdomen (called ascites). The kidneys contribute to ascites by causing salt and water to be retained.
The clot may extend to also block the inferior vena cava (the large vein that carries blood from the lower parts of the body, including the liver, to the heart). Varicose veins in the abdomen near the skin’s surface may develop and become visible.
Eventually, severe scarring of the liver (cirrhosis) occurs.
Usually, the cause is a disorder that makes blood more likely to clot, such as the following:
- Excess red blood cells (polycythemia)
- Sickle cell disease
- Inflammatory bowel disease
- Connective tissue disorders
- Injury
Sometimes Budd-Chiari syndrome begins suddenly and rather severely, typically during pregnancy. During pregnancy, the blood normally clots more readily. In some women, a blood clotting disorder may first become apparent during pregnancy.
Other causes include disorders that develop near the hepatic veins, such as parasitic infections and liver tumors or kidney tumors that press on or invade the veins. In Asia and South Africa, the cause is commonly a membrane (web) that blocks the inferior vena cava. These webs are often present at birth. Often, the cause is unknown
Symptoms vary somewhat depending on whether the blockage develops slowly or occurs suddenly.
Usually, the blockage and symptoms develop gradually over weeks or months. Fatigue is common. The enlarged liver becomes tender, and people have abdominal pain. Fluid may accumulate in the legs, causing swelling (edema), or in the abdomen, causing ascites. Varicose veins may develop in the esophagus. They may rupture and bleed, sometimes profusely. People may vomit blood. Such bleeding is a medical emergency. If cirrhosis develops, it can lead to liver failure. Liver failure can cause deterioration of brain function (hepatic encephalopathy), resulting in confusion and even coma.
Blockages occur suddenly in about 20% of people. Blockages that occur during pregnancy tend to occur suddenly. Some of the symptoms are the same as those of gradually developing blockages: fatigue, an enlarged and tender liver, and abdominal pain in the upper abdomen. Additional symptoms include vomiting and a yellow discoloration of the skin and whites of the eyes (jaundice). Severe liver failure is rare.
Doctors suspect the Budd-Chiari syndrome in people with either of the following:
- An enlarged liver, ascites, liver failure, or cirrhosis when there is no obvious cause, even after testing
- Abnormal results of blood tests done to evaluate liver function plus conditions that increase the risk of blood clots
If results of liver function tests are abnormal, an imaging test, typically Doppler ultrasonography, is done. If results are unclear, magnetic resonance imaging of blood vessels (magnetic resonance angiography) or computed tomography (CT) is done.
If surgery or a procedure to widen a blood vessel or to reroute blood flow is planned, venography is necessary. For venography, x-rays of the veins are taken after a radiopaque contrast agent (which is visible on x-rays) is injected into a vein in the groin.
A liver biopsy may be done to confirm the diagnosis and determine whether cirrhosis has developed.
When the vein remains completely blocked, most people, if untreated, die of liver failure within 3 years. When the blockage is incomplete, life expectancy is longer but varies.
Treatment depends on how rapidly the disorder developed and how severe it is.
Medical Management:
When symptoms begin suddenly and the cause is a clot, fibrinolytic (thrombolytic) drugs, which dissolve clots, help. For long-term treatment, anticoagulant drugs (such as warfarin) are often needed to prevent clots from enlarging or recurring.
Percutaneoustransluminal angioplasty:
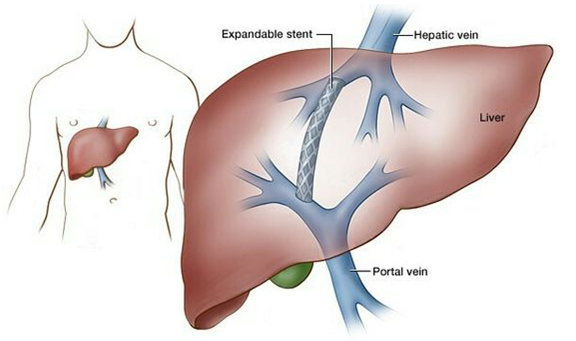
If a vein is blocked by a web or is narrowed, angioplasty may be done to clear or widen it. For this procedure (called percutaneous transluminal angioplasty), a catheter with a deflated balloon at its tip is inserted through the skin into a blood vessel (such as a vein in the groin) and threaded to the blocked vein. The balloon is inflated, widening the vein. A wire mesh tube (stent) is then inserted and left in place to keep the vein open.
Transjugular intrahepatic portal-systemic shunting (TIPS):
Another solution is to create an alternate route for blood flow, bypassing the liver. This procedure, called transjugular intrahepatic portal-systemic shunting (TIPS), reduces pressure in the portal vein. For the procedure, a local anesthetic is used to numb the neck, and a catheter with a cutting needle is inserted into a vein in the neck (jugular vein). The catheter is threaded through the inferior vena cava to the hepatic vein. The needle is used to create a connection (called a shunt) between two veins, usually a branch of the hepatic vein and the portal vein, so that blood can bypass the liver. Then, a stent is threaded to and placed in the shunt to keep it open. The shunt enables blood to bypass the liver, flowing from the portal vein (which normally brings blood to the liver) directly to the hepatic veins (which drain blood away from the liver). The blood returns to the heart through the inferior vena cava. However, such shunts increase the risk of hepatic encephalopathy (deterioration of brain function due to liver dysfunction). Also, shunts occasionally become blocked, especially in people who have a tendency to form blood clots.
Liver transplantation:
Liver transplantation can be lifesaving, particularly for people with severe liver failure.
Problems resulting from the disorder are also treated:
- Bleeding from varicose veins in the esophagus: Several techniques can be used to stop the bleeding. Usually, rubber bands are inserted through a flexible viewing tube (endoscope), passed through the mouth into the esophagus. The bands are used to tie off the varicose veins (termed ligation).
- Fluid accumulation in the abdomen: A low-salt (sodium) diet and diuretics can help prevent too much fluid from accumulating in the abdomen.
Most people need to take anticoagulants indefinitely to prevent new blockages from developing.
