In people with liver failure and cirrhosis, the liver is incapable of processing blood from the bowels. As a result, abnormally high pressure develops within the veins that drain blood from the bowels as the body tries to form other channels for the blood to empty into the main (systemic) circulation. These alternate pathways of blood drainage are known as portosystemic collaterals and consist of fragile veins that surround the esophagus, stomach or other areas in the digestive tract.
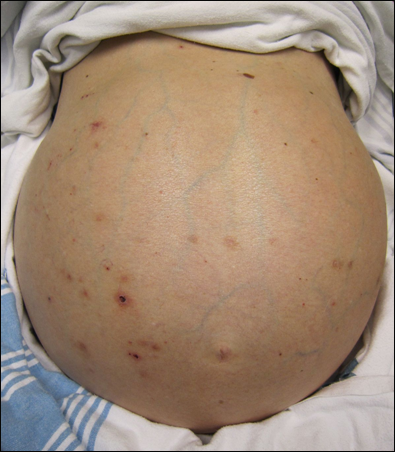
Because of the fragility of these veins, they are prone to rupturing, which can result in massive amounts of bleeding. The abnormally high pressure within the veins draining into the liver (portal hypertension) can also result in the formation of fluid seeping from the surface of the liver and collecting in large quantities in the abdominal cavity. This is known as ascites. Therapies that lower the blood pressure within the veins draining into the liver can lessen the formation of ascites and lower the risk of bleeding from the fragile veins (varices).
A number of therapies can lower the pressure of the veins that drain from the bowel into the liver. The first choice of therapy usually consists of drug therapy with medications known as non-selective beta-blockers. These medications need to be taken everyday to produce an effect. Some people may not be able to remain on beta-blocker therapy if they develop side effects from taking them. Other people on beta-blocker therapy will remain at risk for bleeding from varices and from the development of fluid formation (ascites).
Another approach is to seal off the veins to prevent rupturing. In sclerotherapy, a camera (endoscope) is passed down through the esophagus to inject the abnormal veins with substances that close them off. With variceal band ligation, the abnormal veins are tied off with small rubber bands. Although sclerotherapy and variceal band ligation are very effective in targeting the abnormal and fragile veins around the esophagus, they do not lower the pressure of the blood inside the portal venous system. This portal hypertension may continue to allow fluid to develop inside the abdominal cavity, or may allow bleeding to occur from other areas of the bowel such as the stomach (portal gastropathy).
Pressure inside the portal venous system draining blood into the liver can be relieved by shunting blood away from these veins. Surgical portocaval shunts require an abdominal incision followed by sewing together a portion of the portal venous system to the main venous system. Often these two structures are connected using a short piece of tubing made of Teflon. The surgical shunts are effective at reducing the risk of bleeding from varices. Most surgical shunts will also relieve ascites. The main drawback of surgical shunts is that they are major vascular surgery, and may be associated with a high risk of complications in some patients.
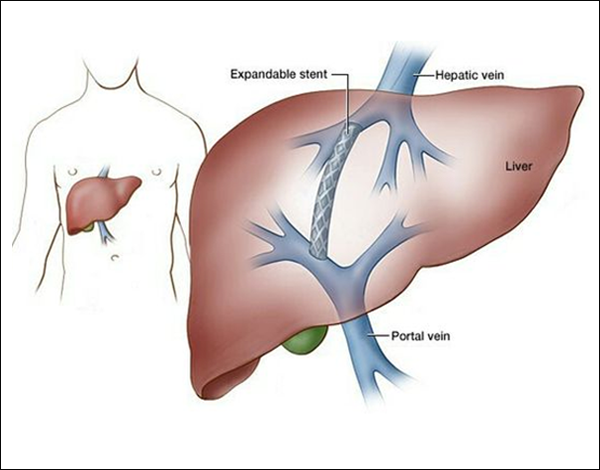
Unlike surgical shunts, TIPS is performed through a small nick in the skin, working through specialized instruments, which are passed through the body using an x-ray camera for guidance. The TIPS procedure creates a shunt within the liver itself, by linking the portal vein with a vein draining away from the liver (a hepatic vein) together with a device called a stent-graft. The stent-graft acts as a scaffold to support the connection between these two veins inside the liver. With the TIPS stent-graft in place, the pressure inside the portal veins is relieved by the blood draining through the stent-graft into the vein draining blood away from the liver.
Over 90% of people that undergo TIPS to prevent bleeding from varices will have a relief in their symptoms and experience little to no bleeding thereafter. When TIPS is performed for ascites, 60-80% of people will have relief in their ascites. Some of these patients will no longer require paracentesis, a procedure where a needle is placed into the abdominal cavity to drain away excessive fluid. Other patients will still need paracentesis, but much less often than before the TIPS procedure. When TIPS is performed for other liver conditions, such as Budd-Chiari syndrome, many patients will have a return to nearly normal liver function once the congested blood drains through the TIPS.
Unfortunately, the TIPS can develop areas of narrowing or blockage within the liver. Usually, these areas can be detected early through regular ultrasound scans performed every three months. Once an area of narrowing has been identified, it can be treated with a balloon to widen the area of blockage (angioplasty). The angioplasty restores normal blood flow through the TIPS. This procedure, known as a TIPS revision, can be performed as a day procedure on an outpatient basis.
Most patients with portal hypertension do not need to have a TIPS. Patients that have esophageal varices and problems with bleeding can often be managed with the drug therapy described above. However, for those patients that continue to be at risk for bleeding or who cannot tolerate the usual first-line treatments, TIPS may be an effective form of therapy. In patients with ascites who continue to form large amounts of fluids within their abdomen, even while taking water pills (diuretics), and who require frequent sessions of paracentesis to drain away the fluid, TIPS may also be a very effective therapy.
TIPS is performed by an Interventional Radiologist. The Interventional Radiologist will determine from your medical history, physical, blood work and liver imaging (CT scans, ultrasounds and/or MRI scans), in consultation with your gastroenterologist, hepatologist, or surgeon, whether or not you are a candidate for TIPS.
You should discuss all your treatment options with your physician. Some questions to ask include:
- Can my portal hypertension be controlled with drug therapy?
- What medications might be appropriate for me?
- If a procedure is required, am I a candidate for a less invasive, Interventional Radiology treatment like a transjugular intrahepatic portosystemic shunt?
- What are the risks and benefits of the treatment plan prescribed for me?
- What are the risks of TIPS?
Because blood that normally flows through the liver gets bypassed through a TIPS, some of the substances absorbed into the body from the intestines can build-up within the blood stream and produce a condition known as hepatic encephalopathy. This is a condition that can affect your brain, causing difficulty in concentration, excessive sleepiness and, in rare cases, a coma.
Most cases of hepatic encephalopathy are manageable by taking a medication known as lactulose. This is a laxative in a syrup form that reduces the amount of certain types of toxins absorbed by the intestines into the blood stream. In rare situations, a person can develop severe hepatic encephalopathy after TIPS. If this occurs, the TIPS may need to be closed off or a smaller stent placed within the original stent to slow down the amount of blood passing through the TIPS. Other risks of TIPS include hepatic failure, bleeding and infection.
Portal hypertension refers to high blood pressure in the liver. One of the major possible complications of portal hypertension is gastric variceal bleeding. Varices are dilated vessels which may rupture, causing variceal bleeding. Gastric variceal bleeding describes the bleeding that occurs when dilated vessels in the stomach rupture, and is associated with high morbidity and mortality rates.
BRTO is a minimally invasive technique that is used to treat gastric variceal bleeding. The procedure involves blocking the dilated vessels, reducing the risk of rupture. It can be used in addition to or as an alternative to TIPS, which is the primary treatment for gastric varices. TIPS aims to relieve the pressure on the dilated vessels by creating new connections between blood vessels in the liver using a shunt.
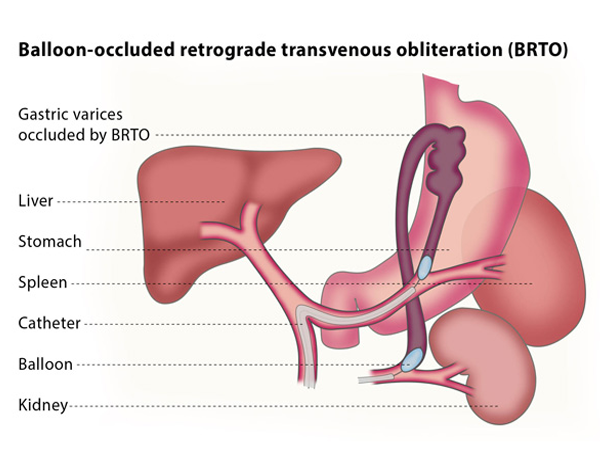
The interventional radiologist will insert a balloon catheter (a thin, flexible tube with a tiny balloon at one end) through a vein in your thigh or neck and guide the catheter to the liver using fluoroscopy for guidance. The catheter is then directed to the gastrorenal or gastrocaval shunt and the balloon is expanded to block the shunt.
The interventional radiologist will then perform a venography, which is a type of imaging technique in which X-rays are used to see the vessels clearly. This will allow the interventional radiologist to confirm exactly which vessels need to be treated and if there are any other abnormal or dilated vessels which have not previously been identified. A medication will then be injected into the dilated vessels through the catheter, until they are completely filled. This medication will remain in the vessel for a short period of time, and will then be removed under fluoroscopy.
Another venography will then be performed, to confirm that the blood flow in the shunt has stopped. Finally, the balloon will be deflated and the interventional radiologist will withdraw the catheter.
You may be advised to undergo this procedure if you are at risk of or already have gastric variceal bleeding and hepatic encephalopathy as well as a gastrorenal shunt. Hepatic encephalopathy refers to the worsening of brain function that is caused by a damaged liver.
Although TIPS has been considered the standard therapy for gastric varices that have been unresponsive to other treatments, recent reports have stated that BTRO is a less invasive and more effective way to manage varices than shunt surgery or TIPS. TIPS does not always cause the disappearance of gastric varices, while BRTO can in most cases completely destroy these vessels.
BRTO has tended to be used to prevent gastric variceal bleeding. It is also an effective therapy for sclerosis (narrowing) of new portosystemic shunts with the additional complication of hepatic encephalopathy. One of the greatest advantages of BRTO is its preservation of liver function. Moreover, the increase of blood flow in BRTO can also improve liver function in cases where the patient has cirrhosis (scarring of the liver).
Procedure-related complications are minor and include bleeding and infection. In rare cases, the blockage of the blood to the gastric varices can further increase the pressure on the liver, causing damage to the liver.
The most serious complications of the procedure, however, are related to the medication used to block the vessels, which is called ethanolamine oleate. Inflow of a relatively large amount of ethanolamine oleate can lead to serious complications. These complications include pulmonary embolism (blockage in a lung’s main artery), fluid in or around the lungs, hypersensitivity, fever, problems with blood flow to the heart and the formation of small blood clots in vessels throughout the body. Ethanolamine oleate also causes haemolysis, which is the rupturing of red blood cells. To prevent this from occurring, only a low dose of the medication is used
The best way to relieve the excessive pressure within a person’s portal venous system is by replacing their liver with a new one capable of filtering the blood. However, many people are not candidates for a liver transplant. The selection process for determining who is a good candidate for a liver transplant may be complicated and require a long period of time. Even in people who are candidates for a liver transplant, less than a third will ever receive a liver; in these people, TIPS may serve as a potentially lifesaving bridge to transplantation while they await the availability of a donor liver.
